In our civilization we have become used to wash and cream our babies several times a day, beginning right after birth. Doing too much, however, frequently results in just the opposite of what actually is intended. The skin cannot develop into a healthy and resistant organ with a well-functioning immune system. Subsequently, the number of individuals with barrier disorders is increasing. Healthy skin is a dynamic system that flexibly adjusts to changing environmental conditions, for instance, it
-
adapts the heat loss to the external temperature;
-
regulates the water loss dependent on temperature and humidity - "under normal conditions" between 0.5 and 1 liter per day;
-
eliminates salts (via sweat glands) and lipid substances (sebum, "lipid mantle of the skin");
-
serves as a barrier against foreign substances and microorganisms including control of the pH level of the skin surface;
-
builds up the individual protection against stress caused by UV-light;
-
protects against mechanical stress; and it
-
transmits pain, temperature and tactile stimuli through nerves.
Frequently, there is also talk of a breathing of the skin. As a matter of fact, carbon dioxide is emitted; however, compared with the lungs, this emission is far below 1 %. Oxygen absorption practically does not occur. Instead, the so-called breathing of skin is rather associated with the unimpeded water loss.
Complex functions
The multi-functional activities of the skin require a complex structure that consists of the following layers: subcutaneous tissue, corium (dermis) and epidermis.
The subcutaneous tissue comprises a loose and lipid-rich connective tissue traversed by major blood vessels and nerves. Its main tasks are shock absorption and heat insulation of the body. The subcutaneous tissue also allows the horizontal shifting of the skin which is a basic function for joint movement.
In the lower parts of the dermis are the sebum and sweat glands with their channels leading to the surface. The dermis is characterized by numerous tiny capillary vessels that transport nutrition and heat. Connective tissue fibers ensure high elasticity and tensile strength.
The epidermis is less elastic than the dermis. It consists of a continuously regenerating surface layer that again is divided into several functional areas. The epidermis does not contain any blood vessels but lymphatic fluid which reaches up to the stratum lucidum (see below). That is the reason why the superficial abrasions that are limited to the epidermis may be wetting but not bleeding. Single nerves end in the epidermis. The epidermal/dermal connection shows tenon-shaped protrusions (papillae), and when these papillary structures form rows they are visible from the outside. These lines are called ridged skin or friction skin; they occur on fingers and feet and determine the individual fingerprint.
Epidermis
Depending on the particular parts of the body, the different skin layers are more or less pronounced, a fact which also applies for parts of the epidermis. The stratum basale, a rather thin layer which borders the subcutaneous tissue, constantly produces keratinocytes (keratin forming cells) including the pigment forming melanocytes. Melanocytes also are found in large quantities on the bottom of the hair papilla; where they release their pigments to the hair that grows at this spot. On their way towards the skin surface, the keratinocytes form the stratum spinosum (prickle cell layer) where their keratinization process (cornification) already begins. Next to it, there are also the antigens forming Langerhans cells which can trigger immune reactions. The cornification culminates in the stratum granulosum (granular layer) where the cells die and mutate into corneocytes (horny cells). This controlled cell death is called apoptosis. The stratum granulosum and the following stratum lucidum are comparatively thin layers. Due to its very densely packed structure, the stratum lucidum (clear layer) forms an effective barrier which is bordered by the stratum corneum (horny layer) with its brick-like structure.
Stratum corneum
The different layers of corneocytes (bricks) in the horny layer are intermitted by lipid bilayers.
Figure: Lipid bilayers (schematized; blue: polar, hydrophilic zones; ochre: lipophilic zones)
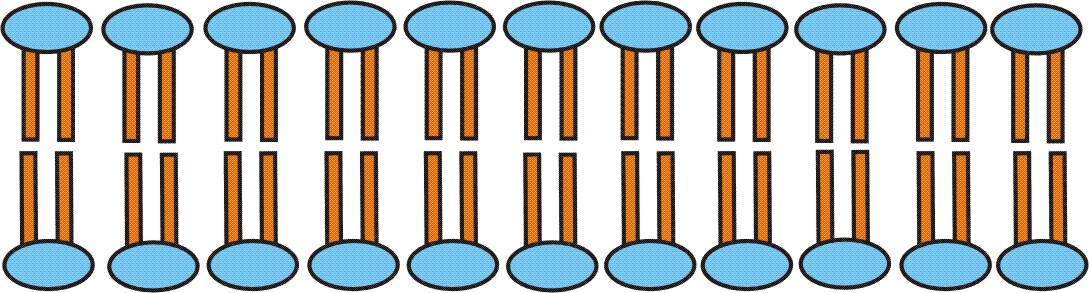
The specific composition of the lipid bilayers consisting of ceramides, cholesterol and long-chained fatty acids largely impedes the penetration of lipophilic as well as hydrophilic substances but also of tiny solid particles. Compared with the deeper skin layers, the stratum corneum is less densely packed. In addition, the skin surface is insulated by lipid containing secretions from the sebum glands. The thinner the horny layer the more translucent it is, while the underlying blood vessels become visible. This applies above all for the lip surface which has neither sebum nor sweat glands.
The flattened corneocytes are interlocked with each other. Furthermore, there are corneodesmosomes in the intracellular spaces. These are macromolecular protein structures that connect the keratinoytes like a network already during their desmosome status and which are strengthened during the apoptosis process. In addition, individual long chained ceramides ensure the cohesion of the lipid bilayers which also are located between the corneocytes. All these different structures added together lead to an extreme stability of the stratum corneum. In case of skin swellings and the related stretching of the intracellular spaces, the corneodesmosomes will suffer and may crack. In particular, high concentrations of hydrogen bond active substances like urea may then cause peeling effects. Enzyme peelings interrupt the peptide chains (see Beauty Forum 2009 (7), 56-58). While these activities only occur in the stratum corneum, fruit acids, salicylic acid and trichloroacetic acid in appropriate high concentrations cause the premature apoptosis of still living epidermis cells through toxic effects; they initiate a removal of these cells and thus stimulate the basal layer to an accelerated regeneration of the epidermis. The epidermis will recover naturally without any external influence within a period of about 2-4 weeks and the horny layer within about 8 days.
Still active...
Although the horny layer is biologically dead, it still fulfills metabolism functions, as for instance through the activity of enzymes. Among these are hydrolases which can hydrolyze triglycerides into di- and monoglycerides as well as glycerin and fatty acids, but also proteases which ensure the supply of amino acids in order to maintain the NMF (Natural Moisturizing Factor) from proteins. The NMF is the most effective protection of the skin against premature aging processes; it moisturizes the skin and is the natural radical scavenger of the skin (see Kosmetische Praxis 2006 (2), 12-14).
The dense population of the skin surface with microorganisms and their specific activity complement the metabolism of the skin. This sensitive balance should not be disturbed by external influences like inappropriate hygienic measures and cosmetic products, among others. Even the horny layer still emits signals that can initiate recovery processes. This specifically happens after barrier damages that increase the TEWL (transepidermal water loss).
Surface active substances like emulsifiers in creams or lotions as well as tensides in cleansing products damage or even destroy the structures of the intracellular areas. Tensides release the lipophilic components out of the lipid bilayers first and then the NMF components which mainly occur in corneocytes. The TEWL increases and the skin dehydrates.
Substance exchange in both ways
The epidermis is a squamous epithelium, or in other words, a sort of covering and closing tissue without a connective tissue or blood vessels. The mucus membranes of the nose, the eye (conjunctiva), mouth cavity and the vagina also are squamous epithelia, although they neither keratinize nor have a horny layer. They are supplied with a liquid film either by their own, or by neighboring mucous glands. Squamous epithelia release substances and can also reabsorb substances from external sources.
The epidermis primarily reabsorbs lipophilic substances that largely migrate into the deeper skin layers via intracellular lipid bilayers and corneodesmosomes structure but also via hair follicles, gland orifices and less frequently via corneocytes. The smaller the molecules the faster they are absorbed. Essential oils, for instance, may already be measured in the blood shortly after their application. This kind of diffusion through the skin is called permeation; while the first step of the process, i.e. the simple integration into the horny layer is called penetration. The more polar the substance the worse it penetrates, which is due to the fact that the lipid bilayers are an efficient barrier. The natural molecules of the skin as e.g. amino acids, short peptide chains or short chained ceramides are different though. With the help of liposomes gained from phosphatidylcholine (PC) which is rich in linoleic acid, it is also possible to transport polar cosmetic agents into the deeper skin layers. In this process, PC fluidizes the lipid bilayers for a short while in order to allow the free passage of these agents. By analogy, lipophilic nanodispersions accelerate the permeation of lipophilic active agents. Since liposomes as well as nanodispersions fuse with the lipid bilayers, the original particles cannot be verified in the horny layer.
Topically applied occlusive substances like vaseline reduce the TEWL. The horny layer swells (see above) and becomes more permeable, a principle which frequently is made use of in topical pharmaceuticals.
In this context, the increasing number of individuals with sensitive skin should be mentioned, who feel a certain burning sensation after the application of O/W emulsions. Closer examination shows that the symptom is not substance induced but rather due to the concentration of polar, water soluble substances in the specific preparation. This particular group of persons generally is characterized by dry skin prone to itching, dilated blood vessels and a weak connective tissue. The idiomatic expression "to rub salt in open wounds" is probably applicable here in this context. Due to the barrier damage that continues beyond the horny layer, the water soluble substances manage to end up in the deeper epidermis layers where their hypertonic concentration can cause major irritations.
Dr. Hans Lautenschläger
Republished: "Brick on brick - the construction principle of the skin, Kosmetik International 2011 (3), 40-43 | 
